Your Guide to GLP-1 & Weight Loss Injections
Ozempic®, Wegovy®, Rybelsus® are the Brand names for Semaglutide
Mounjaro® and Zepbound® the Brand names for Tirzepatide
About the Medications
Semaglutide (Ozempic®, Wegovy®, Rybelsus®) and Tirzepatide (Mounjaro®, Zepbound®) are recommended in the UK for adults as a potential treatment option for weight loss and weight maintenance in conjunction with reduced caloric intake and increased physical activity.
Semaglutide is a Glucagon-like-peptide-1 (GLP-1) receptor agonist that has 94% structural similarity to human GLP.
Tirzepatide is a dual Glucose-dependent Insulinotropic Polypeptide (GIP) and Glucagon-like-peptide-1 (GLP-1) receptor agonist.
In simple words, they are a hormone that activates specific receptors in the body and consequently makes you feel fuller. It is primarily produced by the gut, pancreas and the brain.
What’s the Difference?
Semaglutide gained regulatory approval first, with the brand Ozempic® first to market, followed by Rybelsus® & then Wegovy®.
Ozempic® and Wegovy® are weekly injections where as Rybelsus® is taken as a daily tablet.
The difference is in their licensed use, administration method, and dosage.
Tirzepatide came next, which works on two gut hormones instead of one.
Mounjaro® was the first of this type followed by Zepbound®, both are weekly injections.
There is no practical difference, it is just Zepbound® is the US brand name which is not licensed in the UK.
Wegovy and Mounjaro have become the UK’s dominant brands, mainly due to their specific weight management licenses and NICE (National Institute for Health and Care Excellence) recommendations for obesity treatment.
GLP-1 Patches, you may see these advertised, BUT this is a false association, they do NOT contain actual GLP-1 medications, but rather herbal ingredients and there is no clinical evidence to support their effectiveness in weight loss.
These are unproven and unlicensed products; no clinically approved patch exists to deliver GLP‑1 medications such as semaglutide or tirzepatide, and approved treatments remain tablets or injections.
How Does it Work?
The activation of GLP-1 receptors promotes insulin production by the pancreas, but only when glucose is present in the blood (e.g., after a meal). Insulin is a hormone that lowers blood sugar by helping cells take up glucose, whereas glucose itself is the main sugar found in the blood, not a hormone.
GLP-1 receptor activation also suppresses glucagon release (a hormone that raises blood sugar), slows stomach emptying, and reduces appetite by sending signals to the brain. Together, these effects improve blood sugar control and can contribute to weight loss.
The potential benefits and the risks associated with taking the medication have only been studied in people with increased weight and obesity, who present weight-related issues.
Administration
Prepare
Wash your hands
Check if the medication has a correct label with the name on it
Check if the liquid is clear and not cloudy
Push a new needle every time onto the pen and turn clockwise to tighten
If you use the pen for the first time, turn the dial to two dots and a line symbol
Press and hold the dose button until clear liquid appears at the tip of the needle
Turn the dose selector to the prescribed dose
Inject
Semaglutide / Tirzepatide should be injected into the fatty tissue of the stomach, thigh or upper arm, changing sites of injection each time
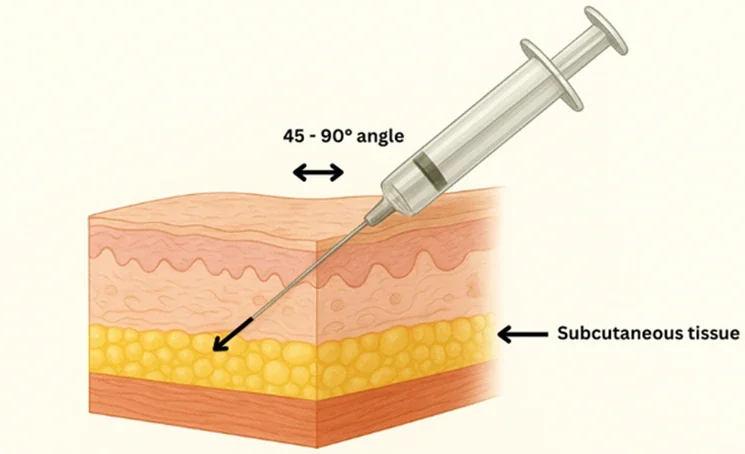
Insert the needle into the cleaned skin at a 45–90° angle into the subcutaneous tissue, and make sure the dose counter is visible
Press and hold down the dose button until the number shows 0, and carry on pressing for 6 seconds after this to ensure the whole dose has been delivered
Potential Side Effects
Every medicine has potential side effects to some degree.
When you first start taking the medication, or at any dose increase, you may experience such side effects.
Common side effects
diarrhoea or constipation
nausea
reflux
vomiting
These are generally not serious side effects and should resolve within days.
However, if the symptoms persist for several days, it may lead to more serious complications, such as dehydration so it is important to stay well‑hydrated by drinking plenty of fluids whilst you are on the medication.
Uncommon side effects
Hypoglycaemia – these medicines can rarely cause a low blood sugar in patients taking them, which can make you feel hungry, shaky and sweaty. Eating or drinking something sugary should stop this quite quickly, but if symptoms persist, medical assessment would be recommended.
Gall stones – again, uncommon but this can cause some right upper abdominal pain and nausea, and needs medical assessment.
Pancreatitis – a very rare side effect, so if there is any severe abdominal pain or upper back pain associated this needs prompt medical assessment.
Lifestyle Advice
Diet
Weight loss injections may influence your hunger levels and digestion; therefore, it is important to focus on the quality of your diet to avoid potential negative effects.
There are three main considerations when it comes to food intake whilst you are on the medication:
Diversity - essential to avoid potential nutrient deficiencies whilst consuming fewer calories
Protein - dairy and lean proteins help prevent potential muscle loss whilst in a calorie deficit.
Dietary Fibre - fruits, vegetables, whole-grains, nuts and seeds. An important source of nutrients which may also help with constipation, a common side effects
Physical Activity
The weekly recommendation for physical activity is to reach at least:
150 minutes of moderate intensity exercise (increased breathing but able to talk), such as brisk walking, swimming or cycling
Or
75 minutes of vigorous intensity exercise (fast breathing and difficulty talking), such as running, playing sports or walking up the stairs
Additionally:
at least 2 days per week should be dedicated to resistance training, which also has a consequent effect on bone density and strength. Apart from weight training at the gym, this can also be achieved by carrying heavy bags or bodyweight training, including yoga.
I’m Sandra, the Nutritionist at Dr Martin – Private General Practitioners
I am passionate about optimising my patients’ health for every stage of life.
Nutrition is a cornerstone of this journey, but to be truly effective, it must be sustainable.
I am dedicated to translating complex science into simple, actionable strategies that respect the importance of enjoying food.
Working closely with our wonderful team of general practitioners allows me to ensure that your nutritional goals are both clinically precise but also fit joyfully into your daily life.
You can read more about me and my approach here in my full bio.
Book your Nutrition Appointment in less than 60 seconds:
Any other questions?
Please do message us below and we will be in touch shortly